Long Covid can take many different forms but fatigue and post exertional exhaustion or malaise is common. As this experience overlaps with ME/Chronic Fatigue Syndrome, pacing is commonly suggested as an option for those with Long Covid.
Pacing is essentially about taking stock of how much energy you have for daily activities and being careful to eke that energy out across the day. Healthy people typically can do anything they want without having to think about the energy required to do them. Long Covid changes things. Everyday things like showering, cooking, walking or driving can cause fatigue. Overexertion or a lack of rest can result in a “crash” where fatigue and other symptoms become overwhelming. Pacing is about avoiding a crash while still maintaining as close to a normal life as possible.
Pacing is not for everyone. Long Covid Physio and World Physiotherapy suggest that pacing may be advisable in the following post-Covid situations:
- People who have post-exertional symptom exacerbation
- People who may have cardiac impairment
- People who experience oxygen desaturation after exercise
- People with autonomic dysfunction, POTS or orthostatic intolerance.
Pacing is seen as a management strategy. It’s something you do to live with a chronic condition. Nonetheless, many people who pace say it has helped them to slowly recover. The focus on rest and avoiding stress may enable the body to improve over time.
Advertisement
The Geek’s Guide To Long Covid is available as an ebook!
You’ll find a comprehensive guide to using wearables, apps and technology to cope with Long Covid. It offers detailed instructions on pacing, heart rate monitoring, HRV, POTS, deep breathing, tVNS, air purifiers, CO2 monitors and lots more.
Available from Amazon
Establish Limits / Baseline
To being pacing, you need to establish your limits and find the “baseline” – how much activity you can sustainably do each day. Long Covid is still a mystery and there’s not a lot of clinical help so the best way to do this is through observation and trial and error.
Observation of the effects of exercise or activity is important to establish how impaired you are. This can be done via diary keeping and the use of apps and devices. As mentioned in Documenting Your Health page, this means keeping track of daily steps, sleep, resting heart rate, HRV and other things, as well as keeping notes on how you feel each day. Comparing symptoms to the previous day’s activities can give an idea of what triggers fatigue and other symptoms.
To get a vague idea of where you’re at, Long Covid Physio recommends the DePaul Post Exertional Malaise questionnaire that asks questions about how often, how long and how severe symptoms after after activity.
Testing of respiratory and cardiac function can help to determine how much pacing is required. A two-day cardio pulminary exercise test (CPET) is an objective measure of illness. It can determine a baseline of activity level and how much it exacerbates symptoms. A CPET typically has the patient perform exercise for 5 minutes while measurements of respiration, heart rate and blood flow are taken. The test is repeated the next date and the measurements compared. A CPET can help identify your anaerobic threshold and the ideal heart rate to stay under if you pace using heart rate monitoring. Unfortunately a CPET can cause a crash afterwards so it should be used with caution.
It’s Not Just Exercise
While we commonly think of “energy” as something we use for physical activity, we also need energy to think, to feel and to maintain relationships. Something as simple as sitting on the couch watching TV still requires mental effort and can be a cause of stress in the body. Talking to people, being in a noisy environment, or feeling stressed or emotional can be draining. When thinking about what has used up your energy during the day, it helps to take account of all factors, not just physical ones.
The Energy Envelope… Or Spoons
Once you have an idea of your baseline, you know how much energy you can safely use each day. Bruce Campbell from CFS Self Help talks about the “energy envelope” and how the challenge is to limit activities so you can stay within your energy envelope. If you live outside the envelope, symptoms will be exacerbated.
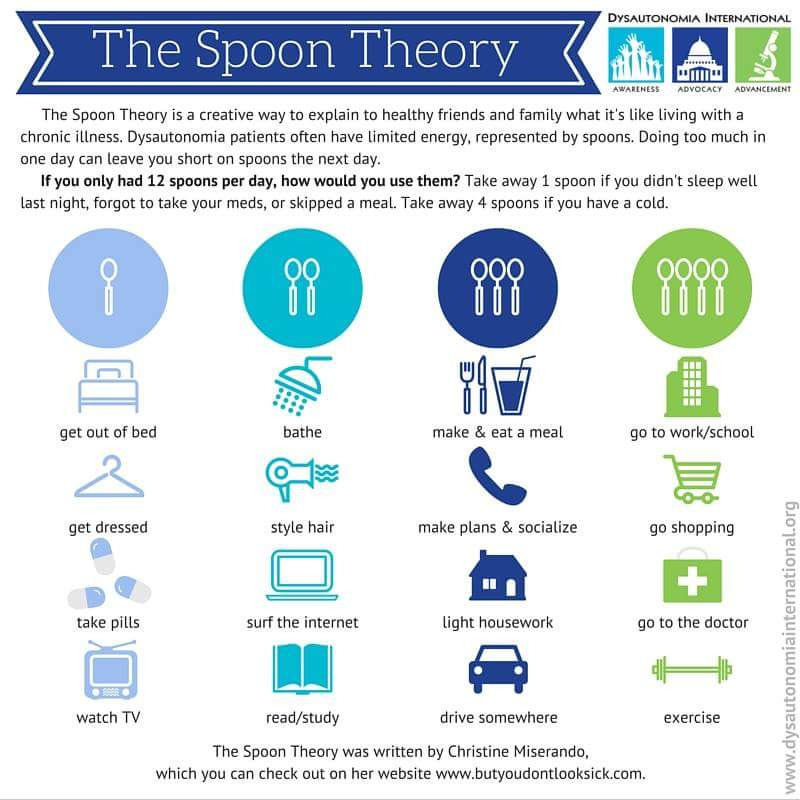
Christine Miserandino from ButYouDontLookSick.com came up with “spoon theory” as a way of describing the process of pacing. Suffering from Lupus, she described her available energy to her friend in terms of 12 spoons on the table. Things like getting out of bed, getting dressed and watching TV removed 1 spoon. Bathing took 2 spoons. More intense activities like shopping took 4 spoons off the table. Every day she had only 12 spoons to choose from and had to apportion tasks according to how many spoons were left. A lack of sleep or illness meant she had even less spoons to begin with. You may see people online saying they “haven’t got the spoons to deal with that”; this is the metaphor they’re using. A bowl full of marbles is a similar metaphor.
Prioritizing Tasks, Setting Limits and Slowing Down
Pacing means making decisions about what is important in your life and what is worth spending energy on. It means apportioning time and effort to things that most matter to you. It means not doing things some days and it means asking for help if necessary. What tasks you prioritize is an individual decision and everyone’s situation is different. You may have people around you who can support you and this can make a big difference.
Setting limits is also important. This means saying “no”, even if you want to say yes. It might mean only spending half the time on an activity than you would prefer. Having set limits means you’re less liable to overdo things and experience symptoms.
One thing most pacing advocates suggest is taking longer to do tasks. This means moving slower, sitting or resting halfway through, and breaking the task up throughout the day. Doing things in shorter bursts means there’s more time for rest. It’s frustrating but it means you’ll have more energy at the end of the day.
It can also help to change the time of day that you do a task. It may be you feel better in the morning and that is the best time to get things done. Again, this will depend on the individual.
Ultimately, you need to reduce your overall activity level, at least in the beginning. This will help you to feel better and be in a more rested state, ready to recover.

Resting
Pacing requires regular resting. This gives your body a chance to recharge throughout the day. Resting can take a variety of forms. It might mean sitting down to perform a task instead of standing. It can mean stepping away and looking out the window or meditating for a few minutes. It can mean lying down with your eyes closed where possible. It can mean a scheduled nap (or two) as part of your daily routine. It also means having good sleep hygiene and sticking to regular bedtimes to ensure you’re well rested overnight.
“Aggressive resting” is a term used by people with ME/CFS to describe the optimal way to recharge, short of sleep. Aggressive resting involves lying down in a dim or dark room with your eyes closed. It must be quiet and non-stimulating; you can’t have music or noise, you can’t watch TV or look at your phone. The only thing you can do is lay there and rest. This gives your brain and body a chance to do very little for a while. This encourages rest and recovery. Aggressive resting can be boring and it’s not how most people would choose to spend their time. For many, though, it’s the best way for them to calm their systems and prevent – or recover from – a crash.
Heart Rate Monitoring
There is a subset of pacing known as heart rate monitoring. This involves keeping track of your heart rate through wearable devices and ensuring your heart rate doesn’t go above a certain rate. It works on the basic idea that a higher heart rate equals more energy used. Beyond that, it aims to prevent fatigue, pain and other symptoms by reducing the time spent above the anaerobic threshold. Read about this in more detail on the separate Heart Rate Monitoring For Long Covid page.
Being Kind To Yourself
Pacing is hard. It puts constraints on your previously free life, it slows you down and it stops you from doing things you want to do. It’s frustrating and it’s depressing. It helps to be kind to yourself and to acknowledge that you’re going through a really tough time. Seek out all the support you need and express your emotions. Talk to your doctor, see a therapist, find a support group online, meditate. Find ways to release the frustration and anger. Remember that stress and negativity also drain your energy but don’t suppress it. Ultimately, you are pacing because you want to stop being ill – whether that means management or recovery. You are looking after yourself first and foremost. Acceptance of your new circumstances is difficult but embracing the change can help you move towards recovery.
Pacing and rest have been recommended as the main thing helping many Long Covid people to recover (see this survey). Pacing helps people to rest and allows your body time to heal itself. If done early, it improves overall outcomes. Remember that this isn’t forever. Keep hoping and keep resting. You’ll be OK.

